April Showers Bring May Flowers – or so the saying goes.

April focused on social distancing, with stores still closed and quarantine still in effect to keep everyone safe until late May. And May has included rain, which brings me migraines, and it has included spending my days on the phone with the VA, so nothing new.
With my last blog post, March Madness, I touched base on all of my problems and how this COVID chaos is changing the way I see my health care teams.
I know my rheumatology clinic visit was changed to a phone call consultation, my hand specialist appointment, too. My physical therapy visits have been done virtually, with no in-person appointments being rescheduled until the risk of getting sick is brought down.

So, my quarantine has included a lot of baking (my love language), listening to vinyl, finding four leaf clovers, and, just trying to take care of my body during these times of crisis. Quarantine isn’t very hard for me, I am used to staying home in pajamas and social distancing with fears of getting sick. This isn’t anything new for the chronic illness community.

But, even though the world stops for quarantine – for the most part – it doesn’t mean our problems stop, and we have to continue to self advocate and seek care when our bodies are not being nice.
So, let’s begin with everything in my life that is not rib related.
- Crohn’s Disease
The day after I posted March Madness, I had an update to my pill capsule endoscopy for my Crohn’s disease available on myHealthevet, my online health record with the VA.
Normal bowels for the most part, with some ulcerations but no bleeding seen. I haven’t followed up with my GI yet, but I am expecting her to tell me that I am in remission with my Crohn’s disease while using Stelara.
This is the first time I have even been close to remission, although I have been on a mission for remission for 6 years now. This means my Stelara medication is working and that with proper maintenance, I can hopefully see fewer problems with my Crohn’s disease and I can focus on trying to avoid flaring rather than fighting active disease.
Now, this does not mean I am symptom-free. While also having IBD, I mentioned that my GI told me that I could be suffering from other issues as well as the Crohn’s disease.
Now, I was supposed to have a follow-up with my gastroenterology care team but the COVID chaos has prevented me from going to the VA and getting the care I need. With every appointment canceled and no end in sight, my GI appointments have turned into phone call check-ins and suggestions over the phone.
Since I still have a few symptoms with my Crohn’s disease and my Stelara levels looking okay, we are adding Immodium to my medication list, to see if it helps and of my issues. I did ask for photos and images from my pill capsule but my GI told me that I would need a specific program to view the pill capsule data, so not getting anywhere with that request. I will have her pull up the files on her computer during my next in-person visit so I can grab a few cell phone photos to share.
I have a virtual appointment with GI on May 19th, which happens to be World IBD Day, which seems fitting for the day I speak to my GI care team and update them on how my body and IBD is managing. I will be getting another check-in phone call from her in a few weeks and hopefully, things will get back to normal after that.
- Physical Therapy and These Ribs
I know with physical therapy, all of my current and future appointments have been set up for virtual meetings. I have done a few meetings with my care team but I am not currently doing physical therapy exercises anymore.
I am still having issues with my ribs. I know, I know.
But, to be fair, I am only 3 months post-op – having just had my chest wall opened this past January for the third time. Some days I over-do it, some days I hurt more than others. I am trying to heal but my body continues to fight me.
I have been having problems with slipping rib syndrome as well as issues with my previous surgery scars. It has been almost a year and a half since my neurectomy surgery and I have already gone through two infections and opening the incisions back up. Now, it is getting bothered again.
This time though, it is the incision below the problem incision from last year – there are 4 incisions from that surgery, number one had problems last year, number two is problematic now.
In addition to that incision being bothered, my incision from this past January’s rib plate removal and rib resection surgery, it has gotten inflamed, too. The incision was looking healed, with no redness or swelling, but now that I already have inflammation on that side, this incision has decided to join the revolt against my left side.
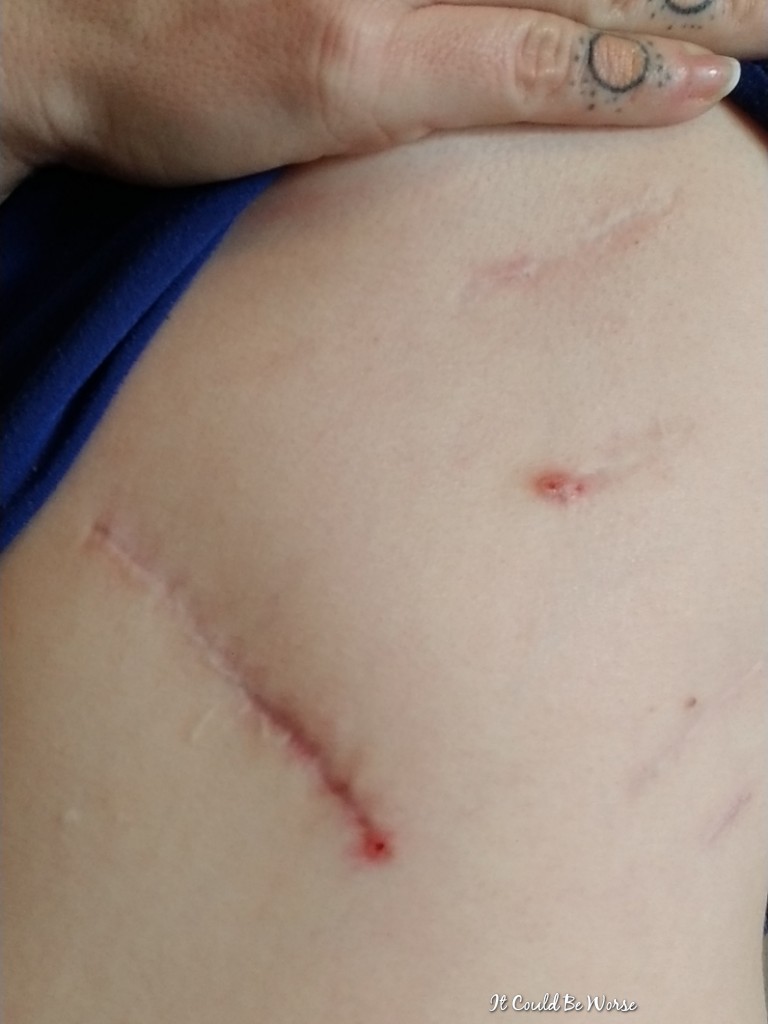
So, instead of one wonky incision getting irritated, I have two.
Now, the wonky rib that was slipping, the one that we plated and ended up removing the plate from, with a resection of a portion of my 10th rib, that area is still problematic. I feel pain and pressure at my 10th rib and I have been living with the fear that my 11th rib is now slipping under my 10th rib – the same issue as before, just one rib down.
I know I have read about slipping rib patients having bilateral surgeries and some have multiple surgeries for ongoing slipping ribs, but I cannot seem to get a break in all of this. If this rib is slipping, we are back to square one. I doubt nerve blocks will help – they don’t help bone on bone grinding, and when I research I find that eventually, this 11th rib tip will have to be stabilized or resected, too.
To say I am beyond exhausted is an understatement. I think back to a few years ago, before any rib issues, and I think about how nice it was to get dressed with no pain, bend over with no pain, and how nice it was to move without pain. I haven’t had a day without pain in a long time, it has been years.
I had tried calling my cardiothoracic surgeon in mid-April, leaving multiple messages for her to return my call so we could talk about these open incisions. I know the VA is not seeing patients right now, but a return call would be appreciated, considering I am fighting another slipping rib and I currently have incisions that are fighting infection after a year of being okay. I would love to just let her know about what is going on, I had already filled in my physical therapy team and we are taking it easy until I finally got my surgeon on the phone.
I had to wait over two weeks from the first time I called to speak to anyone about my ribs. You would think they would want to contact me and help me prevent further infections, pain, and other ribs slipping. I am avoiding my therapy exercises to prevent further bone on bone grinding in my ribs.
I am constantly stretching out my torso trying to relieve the pressure in my xiphoid process and at my 10th rib tip and costal margin.

The compensating for these ribs has caused me pain in my back, I have been sore at my left hip, my knees and even my shoulders have been sore. My body is fighting the pain, I am constantly correcting my torso, and that is causing my body to be sore and fatigued all of the time. I do not sleep well, I toss and turn all night. I usually wake up in pain from trying to sleep on my right side – not the surgery side – but even laying on the opposite side leaves me feeling like my ribs are collapsing and there is pressure in my left side ribs if I try to lie that way. I can feel my 11th rib slipping under the 10th if I lie on my side, and if I lie on my back, I can feel the 11th rib touching my 10th rib. I spend all day trying to avoid the rib-on-rib touching and slipping. IT IS EXHAUSTING.
So, I finally had an in-person appointment scheduled. After no return calls from the cardiothoracic clinic, I spoke to my primary care team nurse and she put in urgent notes for them to contact me – she knows I have been dealing with these ribs for a long time and she trusts my judgment that when I say I need to see someone or speak to someone, that I am usually right when it comes to my body. They trust my judgment when it comes to going to the ER, getting sick, and other things because I am rarely wrong – I know my body pretty damn well after being on constant alert with it for the last 6 years.
Funny, not five minutes after my primary care phone conversation, I had a call scheduling me with my surgery team the next day. It only took two weeks and a push from other clinics, but I did get seen. I was safe, I didn’t touch anything, and I made sure to wear my mask that my twin made me.

With that visit, I mentioned the inflamed incisions. I mentioned the pain in my 11th rib. I mentioned that it is causing constant pressure and that the 11th rib is slipping under the 10th rib, just like my 10th rib would do before it was sutured back into its correct place.
My surgeon said I have suture granulomas, little areas of inflammation where my body likes to reject stitches. She told me it was a positive thing that they were not infected, that she would go into the incisions and remove the sutures that are causing problems and close me back up. This would be a minor surgery but I would need a little anesthesia for, and she planned that for early this June once clinics are fully opened.
Because one of my incisions is over a year old, that means that there is a reaction to the suture materials – like last year, my body rejected multiple stitches during their bouts of infection – I remember stitches coming out after one incision burst on me. My body does not like stitches, even the ‘dissolvable’ kind. We would leave these sites alone, but since they started getting inflamed on their own, we want to remove the small areas of the wound sites before they get infected.
As for the pain, I felt a little blown off about my 11th rib slipping. I know that in January, my ribs seemed like they would heal and the slipping of ribs would be done. But now, at three months post-op, my body is shifting/has shifted into its ‘new normal’ position, and my 11th rib is shifting upward toward the rest of the above ribs.
With my body and posture compensating for these ribs for so long, my torso has shifted and my spine has moved. It makes sense that the 11th rib is moving, too, and that we have to take these adjustments as they come.
My surgeon suggested getting yet another CT scan and referring me to the pain management clinic for nerve blocks to help the pain caused by the intercostal nerves being bothered. But, to be fair, I have had nerve blocks, I have had a few of them. I have had neurectomy surgery, for nerves 8 through 11 but nerves can grow back, apparently, so I find that by not fixing the mechanical issue, I will continue to have bone on bone grinding in my ribs.

So, I will get the CT scan. And I will show up for the suture granuloma surgery. But, I did try calling my cardiothoracic care team back and left another few messages with them, letting them know that after a few days of dwelling on my previous appointment, that we needed another conversation about this 11th rib slipping.
I know I mentioned it to each clinic, the bone on bone grinding, as I have to self advocate when I have gone through this before. I do not want another year to pass and the only help I can get is nerve blocks when I know there is rib-on-rib grinding.
I did have yet another physical therapy virtual session and I filled in that clinic’s care team about what is going on with these ribs, too. She agreed with me about fixing the mechanical issues versus focusing on pain management first, as she knows I have lived through this before. I was released from the physical therapy clinic, as there is not much she can offer until my pain with these ribs has quit. I can continue to stretch as much as I can but for now, I will no longer see that clinic.
I have been scheduled for a consultation with the pain management clinic later this week and I made sure to mention my 11th rib and discussing things with my surgeon first, too.
And, to my surprise, my cardiothoracic surgeon reached out to me sooner than I thought they would about my concerns about this 11th rib.
My surgeon called me and I tried my best to fill her in about this rib – the grinding, the feeling of the 11th rib tip going up and under my stabilized 10th rib, that I feel a nerve block would help, yes, but only temporarily, and that we needed to have another talk about our plan.
Luckily, my surgeon understands my problem and appreciates everything that I have to go through to get my body right.
The plan as of now is to go ahead with the CT scan – as I had planned – and to go ahead with the pain management consultation that will be done virtually this week – as I had planned.
She did mention that if her clinic and the pain management clinic decides that my rib is slipping after seeing my CT scan, then I may have to go in for another titanium plating procedure to secure the rib and prevent it from slipping up and behind, or I may have to have it stabilized with sutures like my previous slipping rib.
Either way, I know the plan is not ideal but I cannot have this slipping rib for the rest of my life.
I will speak with her next week and we will come up with a definitive plan.
After that, I finally have a video appointment with my hand specialist about my De Quervain’s tenosynovitis. I mentioned it in my March Madness post, that my right hand being used so much has started to inflame my tendon sheath and that my left was healing from the tendon sheath surgery performed on that one. I will discuss wearing my braces this year and the pain that I get in my right wrist. If I can get this hand under control, then my hands should have no further issues as long as the cysts in my hands stay small and not bother me.
So, we have a plan for these ribs, so far, with another phone call planned next week.
I have fought migraines all week, so that will be something to mention when I follow-up with neurology.

I have a plan with GI and my follow up call scheduled for later this month before Stelara self-injection #15.
I have a plan to speak with my hand surgeon next week after speaking with GI.
I think I have it all covered?
It is a lot to deal with and I know it could be worse so I will end mentioning my previous post about Gali Health.
I have been asked to be one of Gali Health‘s newest Ambassadors! I needed this good news today, for sure.

3 Months Post-Op Slipping Rib Syndrome 
3 Months Post-Op Slipping Rib Syndrome
I will write articles and share my patient perspective, while also trying to help others in their IBD journey.
To learn more about Gali – see my post Gali Health Ambassador.
Until next time, for me, It Could Be Worse.

Thank you for reading, and for keeping up with My Crohn’s Journey.Please “Like” It Could Be Worse Blog on Facebook!
And as always, any information you’d like to offer up about Stelara or any of my current struggles and/or issues, I have open ears and I’ll happily take any tips you have to offer!
CURE for IBD: For those of you who are continuing to donate to the Cure for Crohn’s and Colitis, I encourage you to donate towards my team page with CURE for IBD – where 100% of the funds WE raise will be allocated to IBD research for a cure. That’s right, 100%!!
To Donate: www.cureforibd.donordrive.com/campaign/icbwblog
Previous Posts on It Could Be Worse:


