Thoracic
Thoracic seems to be another clinic that I frequent. I have suffered from rib pain for about a year now. Sudden onset of pain, with two major areas of focus on my left side. We are not 100% certain that these pains are related or not.
Because there is so much to cover in the last few months, I am separating one long blog post into multiple postings. And, since my ribs and surgery had become a whole ordeal, it gets its own post about the events of that. There will be more postings within the next few days, this one just happens to be finished first.
Warning – there will be photos of my incision site and healing process.
As I have mentioned many, many times, I have wonky ribs.

The first problem, I have a single swollen rib on my side/back area. We think this is my 10th or 11th rib, with one area that is significantly larger than the rest that would get inflamed.
When I say inflamed, I mean it was one general rib, in one general area, that would swell and become painful to the touch. This one rib area was almost as if the cartilage at the end of one of my floating ribs was swelling or becoming irritated.
To help this, we had done a temporary nerve block, numbing the area for a small time. If you remember, we had discussed a neurectomy before the nerve block, but, after, my doctor was too ‘hesitant’ to do what we had discussed. I was referred to Rheumatology, given a rib binder, and told to wait a month and return. See One Step Forward, Two Steps Back.
When I returned, this appointment was a hot mess in waiting. I had arrived for a 9:45AM appointment, waited for over two hours before they told me I was actually rescheduled for 1PM, and even then I had to wait until after 2:30 to be seen.
And then…the doctor was still extremely hesitant about removing the problematic ribs and nerves, so he wanted to ‘discuss my problems with other surgeons’. This meant more waiting and another appointment scheduled. I was told to wait another two weeks and return. Why wasn’t this done during any of my week-long waits for these appointments? It just doesn’t make sense to me.

When I returned for the latest in my thoracic visits, I was told a neurectomy and rib resection was in the works. I was surprised and given another temporary intercostal nerve block, this time with Lidocaine and without a full on “surgery” planned.
The thoracic intern numbed me up as I was half-sitting, half-laying down with my shirt pulled up. I had my hands placed at the beginning and end of the specific rib swelling, giving her an idea of which rib and nerve area to target. The numbing portion of the procedure is the worst part, the lidocaine burns a little and I wasn’t completely numb before she attempted another needle insertion.
Moments later, I was numb.
They had me sit for a moment and then felt around on my rib area to confirm that this nerve block helps the feeling go away in this rib swelling, which it does. I was completely numb on that one targeted area, if only it helped the second issue.
The second issue, the rib popping sensation, I have in the front of my ribs below my breasts, it occurs more and more and more. One of my front ribs is rubbing up against another, moving forward and behind the rib above it, causing pain and a sickening feeling as it happens randomly as I move.
If I sit, I can feel it. If I turn my sides, I can feel it. I feel it driving, I feel it laughing, I feel it coughing or sneezing or bending over. The brace stabilized the area, but it does not take away the rib grinding sensation completely.
I have tried to research the hell out of this, and, to the best of my knowledge, it is called Slipping Rib Syndrome. With some research, it is in my opinion that this rib problem is also the culprit for problem one, as well. I have read that Slipping Rib Syndrom can lead to intercostal nerve problems, swelling and pain, which are exactly my current issues.
Now, Slipping Rib Syndrome (SRS) is usually only found by hook-maneuvering the ribs in the affected area, feeling for the movement and friction of the touching ribs. X-rays, MRI’s, ultrasounds, these are not necessarily the best for viewing SRS, and it may show absolutely nothing. So, I had all of these procedures done, potentially for nothing if I am correct. And I assure you, I am 99.9% sure I am. You can see my video of my own ribs here.
In researching this, a rib resection of the affected areas is usually the best plan of action. Funny, I have been suggesting this to the doctors since early May of last year, to which the doctors took as “asking for surgery” rather than me knowing what my body needs to get rid of the pain.
Lest they forget, I am the one living and breathing in this body. I know when something is wrong.
Now, I have been seeing the Thoracic clinic for over a year due to the two main issues with my left side rib and chest wall.
Remember, we did temporary nerve blocks to this area, and after a day of relief, we knew from the get-go that a neurectomy would help. But, things aren’t as simple as that.
After seeing the thoracic clinic and discussing how the nerve block worked for temporary relief, my surgeon was still hesitant, if you remember, and he wanted the second opinion from some of the other doctors I see, such as rheumatology.
After seeing rheumatology, and seeing the thoracic clinic numerous other times, wearing the rib binder, etc., I was still suffering from problems one and two. Even months later.
Problem two, that slipping rib in my front left side rib. Around my 9th or 10th rib, one rib ‘pops’ or rubs up against another rib above it. This sensation is extremely uncomfortable, with the popping becoming easier and easier to replicate and reproduce, usually to show others that I can INDEED feel the rib slipping.
Now, my thoracic surgeon refuses to acknowledge this issue, saying I have asymmetry in my costochondral and front rib area cartilage. The surgeon refuses to acknowledge that he can feel the popping sensation when I have showed it to him, when others I have shown can feel it as well.
So, after months and month of visits and nothing helping the problems, the neurectomy surgery was a go. No resection, just permanently cutting nerves.
January 23rd, I went into the thoracic clinic with expectations of a few, possibly two, small incisions to cut the nerves below those problematic ribs.
It took two stabs to get my IV started, which usually seems to happen when I go in for surgery, and, I had the IV placed on the back side of my arm, which was new to me. I was given fluids, marked on the left side of my body where the incisions would go, and I was given happy meds to go to sleep.
When I woke up, things were a little different than what I had been told would happen.
When I woke from surgery, I remember being extremely sore and nauseated. I tried to look at my side where the surgery was, but there was gauze dressing covering it. There was also a tube running from inside of my side, with a blood-filled grenade ‘thing’ attached to it. Pneumothorax or chest tube is the correct verbiage, but for me, I’ll keep calling it the blood grenade.
I was told that there were four incisions made, with the lowest incision being the tube leading to my lung, which was collapsed during surgery. I was told that I was expected to stay overnight, which was news to me. I told them I had intentions of going home, same-day, and so they called my surgeon, who had already left for the day, to get confirmation that I could leave.
At first, the plan was to leave the tube inside of me, and that we would remove it the next day. The nurse was instructing me on how to drain the blood-grenade thing and I was okay to go.
After speaking with my care team, they decided that we could remove the tube and let me breathe a little while before getting an x-ray, just to make sure everything was okay on my insides and that my lungs fully expanded back up. Below is a comparison of my x-rays, before and after surgery.

The after-surgery care team removed my tubing, I had to sit up, drink something and snack on something before I could leave. I remember projectile-vomiting as soon as I stood up to get dressed, so the nurse gave me more anti-nausea in my IV before removing it. The apple juice they gave me to snack on was too sweet, the crackers too salty, so I was ready to leave and get coffee immediately.
I was given pain medication, extra gauze dressing, and sent on my way. I was extremely sore, I felt like I could not catch my breath after the collapsed lung, and I could barely move from the pain and tightness. After surgery, all I wanted to do was sleep but even laying down was a whole ordeal.
Coughing, sneezing, and laughing has been brutal on my chest wall for the last two months since this surgery. Every movement that involved the rib or chest wall, I definitely felt pain.
After I got home, I could see the incisions and surgery area. I had one special dressing over the hole in my side from the tubing, and it was traumatizing to see, especially seeing on my own body.
After the surgery, the next day I was to change my dressing. I went out to get coffee, to see how I felt driving, and on my way, the plastic bandage had burst, which ruined the pajama top I was wearing. With the dressing change, it meant I could see the damage.
The next few weeks were pretty brutal. I was in some severe pain for days on end, and, of course, allergies got to me, causing me to sneeze more, ouch.
And, I am pretty funny and I love to laugh, which, in turn, hurts. The more I tried not to laugh, the harder I had to fight laughing more to avoid pain. Every giggle, I’d have to hold my chest wall and try to hold on my laughter.
The first three weeks after surgery was pretty bad, I never knew how funny I could be until I wasn’t able to fully laugh. Hell, even my laugh changed there for a few weeks, with the collapsed lung healing and my chest wall being so tight and unmoveable. The new laugh was almost fake sounding, I was afraid I was going to be stuck with it forever.

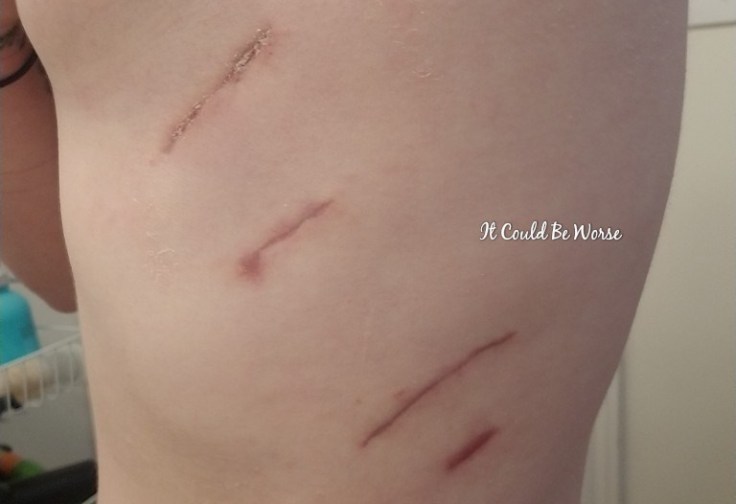
But, I can’t feel the front portion of my chest wall anymore. During surgery, they cut my 8th, 9th, 10th, and 11th rib nerves! I will never have feeling in this area ever again.
It was pretty wild at first when I would shower, there would be a clear line of demarcation where the feeling area met the non-feeling area. After I would shower each day, that numb area would be a bright shade of pink and red, but only on the area affected by the neurectomy.

Around three weeks after surgery, I started running a fever of about 100.7. Then, my fever spiked to over 101, so I called the VA triage line so that I could speak with a nurse.
At this point, my top incision was the only one not healing fully. The lung collapsed tube hole, I would have thought it would be the problem area, but the top incision was just not healing.
Where the top incision sits, it is right underneath the side of my left breast, with my breast touching the incision at times. This incision started to swell, getting hot to the touch, turned red, and even began to swell the bottom of my left breast.
When I looked at the swelling, it had a significant area of inflammation going on, over the incision itself and spreading infection in my breast at this point. The VA emergency room triage nurse recommended going into the ER for a visit, to get started on antibiotics immediately. I was told that because I was taking Tylenol for the past few days, my fever was probably higher than the 101 my home thermometer was telling me.
I went into the ER and was seen by one of their care teams. was told to look out for an abscess or draining, and to return if it got worse or I hadn’t broken the fever. I was given antibiotics, Ciprofloxacin, and sent home early in the morning.
By the next night, my incision had opened itself slightly and was draining the infection. I returned to the emergency room and was told that I was going to have to get the inflamed incision reopened and drained. I was in tears but I knew I had to have it drained.
The ER surgeon gave me a few Lidocaine injections near my incision, which hurt even more when the Lidocaine starts to burn. Ouch.
Once I was numbed, she cut two areas open and I could feel the fluid draining down my back. I could tell immediately that my breast was getting back to normal, they packed and dressed my new incisions, and I was told to return the next day for a dressing change.
Notes were sent to my thoracic surgeon both nights at the emergency room, with notes for them to see me if available and to redress my incision in the clinic. I was also told that if he could not do it, then I could return to the emergency room to have it redressed as well.
The next day, I had an appointment with GI for my Crohns disease, but the thoracic clinic is in the same area at the VA. I tried to be seen by my thoracic surgeon, especially since I had been to the ER twice in the last two days, but I was told that he was ‘too busy’ and could not see me. Not even for two seconds to look at my incisions.
So, I went back to the emergency room and had them redress my incision and remove the packing. I had to be checked into the emergency room for the third time in three days, which is never fun. But they told me that I was complicated, so I needed to be checked in rather than just popping in to have my incisions cared for.
Once they redressed my incision and removed the packing, I was sent on my way, again. Talk about deja vu.
After that last emergency room visit, I have seen thoracic since then, and my incisions seem to be healing, finally. That top incision is almost fully closed, at a month later, and there is only a very small hole still there. I only notice it when the incision is wet, so I try to keep an eye on it.
The last thing I need is another infection and more problems with this rib area.
I believe with my already compromised immune system, and since I had just had surgery before this rib surgery, in October for my hand, that my body was just not prepared, so it fought against itself.

I was trying to work a lot, go places, still attempting photoshoots, and everything else. I needed to take it easy to prevent the infection. I had thought I was good to go after a month of healing but my body needed more time to heal.
I am doing much better since those last doctor visits, and I will be following up with my thoracic surgeon this week, actually. I can still ‘feel’ the popping, but there is not any feeling to the area, with my back rib not painful to the touch. So far, as long as the slipping rib isn’t causing issues and I cannot feel it, I am managing.
I have begun having movement with this side, I can actually sleep on my side now, which was difficult to do at first. I can laugh and sneezing is still a bitch, but I’ll get there.
I will be following up with a few other blog posts, specific to my Crohn’s and my Stelara, and everything else.
Until next time, for me, It Could Be Worse.
————————————————————————–
Thank you for reading, and for keeping up with My Crohn’s Journey. Please Like It Could Be Worse Blog on Facebook!
————————————————————————–

And as always, any information you’d like to offer up about Stelara or any of my current struggles and/or issues, I have open ears and I’ll happily take any tips you have to offer!
————————————————————————–
CURE for IBD: For those of you who are continuing to donate to the Cure for Crohn’s and Colitis, I encourage you to donate towards my team page with CURE for IBD – where 100% of the funds WE raise will be allocated to IBD research for a cure. That’s right, 100%!!
To Donate: www.cureforibd.donordrive.com/campaign/icbwblog
————————————————————————–
IBD News Today Column:
Welcome to ‘It Could Be Worse’ – A Column by Mary Horsley————————————————————————–
Previous Posts on It Could Be Worse:
Two Months Time | IT COULD BE WORSE BLOG
Stelara Self-Injection #2 & Rib Pain
Lumpy, the Ganglion Cyst, a Trilogy
Stelara Self-Injection #1 | It Could Be Worse Blog
2 Year Anniversary of Crohn’s Diagnosis Day | It Could Be Worse Blog







































